Untangling NICU Care
Soft, flexible wireless sensors allow parents to hold their premature babies.
When Taschana Taylor underwent an emergency c-section, her premature daughter grace was rushed to the neonatal intensive care unit (NICU) and remained there for weeks.
Once Taylor recovered and was able to see her daughter, she encountered an unexpected obstacle: the cumbersome bundle of wires connected to sensors on Grace’s body to monitor the baby’s vital signs —heart rate, respiration rate, and body temperature.
“Trying to feed her, change her, hold her, with the wires was a little contained,” Taylor says. “If she didn’t have the wires on her, maybe we could go for a walk around the area. Maybe we could probably spend the night upstairs together. It would have made the entire experience more enjoyable.”

Listening to Mother
For years, a Northwestern University team co-led by a Northwestern Engineering researcher has been trying to solve this problem by developing wireless sensors that would allow a greater range of movement and interaction with newborns. The team came up with a pair of soft, flexible wireless sensors that work from opposite ends of the baby’s body. One sensor lays across the chest or back, the other wraps around a foot.
While existing sensors must be attached with adhesives that can scar and blister a premature newborn’s skin, the wireless sensors feature patches that use much weaker adhesives. “We wanted to eliminate the rat’s nest of wires and aggressive adhesives associated with existing hardware systems and replace them with something safer, more patient-centric, and more compatible with parent-child interaction,” says John A. Rogers, a wearable electronics pioneer who led the technology development.
This spring, the team completed the first human studies using the wireless sensors on premature babies at Prentice Women's Hospital and Ann and Robert H. Lurie Children's Hospital of Chicago. Taylor’s daughter Grace was among the 70 babies who wore the wireless sensors, which, for the studies, were used alongside traditional wired sensors. Having both sensors allowed the Northwestern team to compare the data collected from both types.
“When we were approached about the study, Grace’s father and I were really excited,” Taylor says.
The studies revealed that the wireless sensors provided data as precise and accurate as that from traditional sensors. “We were able to reproduce all of the functionality that current wire-based sensors provide with clinical-grade precision,” says Rogers, Louis Simpson and Kimberly Querrey Professor of Materials Science and Engineering and Biomedical Engineering in the McCormick School of Engineering and a professor of neurological surgery in the Feinberg School of Medicine. “Our wireless, battery-free, skin-like devices give up nothing in terms of range of measurement, accuracy, and precision — and they even provide some additional measurements that are clinically important.”
"We know that skin-to-skin contact is so important for newborns - especially for those who are sick or premature. When you have wires everywhere, and the baby is tethered to a bed, it's really hard to make skin-to-skin contact."
Encouraging Parental Bonding
The mass of wires that surrounds newborns in the NICU is often bigger than the babies themselves. Typically, five or six wires connect electrodes on each baby to monitors for apnea, blood pressure, blood oxygen, and heart rate. Although all those wires help ensure health and safety, they constrain the baby’s movements and create a major barrier to physical bonding during a critical period of development.
“We know that skin-to-skin contact is so important for newborns — especially for those who are sick or premature,” says Amy Paller, Walter J. Hamlin Professor of Dermatology and professor of pediatrics at Feinberg as well as a pediatric dermatologist at Lurie Children’s Hospital, who jointly led the research. “It’s been shown to decrease the risk of mortality, infections, pulmonary complications, and liver issues, and to increase the baby’s ability to gain weight. When you have wires everywhere, and the baby is tethered to a bed, it’s really hard to make skin-to-skin contact.”
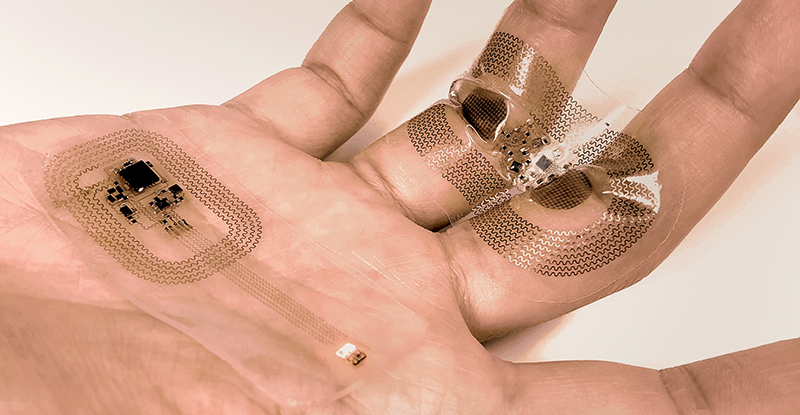
The benefits of the Northwestern team’s new, small technology — the chest sensor measures 5 by 2.5 centimeters; the foot sensor is 2.5 by 2 centimeters — reach beyond its lack of wires. The dual-sensor system allows physicians to gather an infant’s core temperature as well as body temperature from a peripheral region.
“Differences in temperature between the foot and the chest have great clinical importance in determining blood flow and other aspects of health status,” Rogers says. “That’s something that’s not typically measured today.”
Filling in Information Gaps
Physicians also can measure blood pressure by tracking when the pulse leaves the heart and arrives at the foot. Currently, there is no good way to reliably measure blood pressure on infants. A blood pressure cuff can bruise or damage fragile skin. The other option is to insert a catheter into an artery, which is tricky because of the narrow diameter of a premature newborn’s blood vessels.

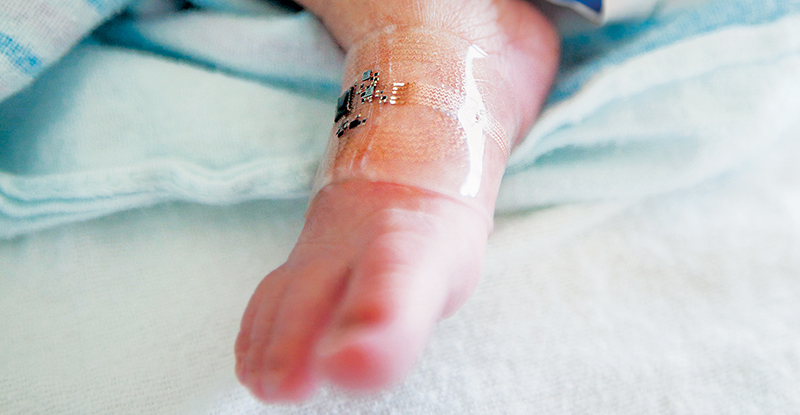
The new device could also help fill in information gaps that exist during skin-to-skin contact. If physicians can continue to measure the vital signs of infants being held by their parents, they might learn more about how critical such contact might be.
Because the sensors are transparent and compatible with imaging, they also can be worn during x-rays, MRIs, and CT scans. “Wires are not just a physical impediment to interacting with the baby, they also disrupt imaging if left in place,” says Paller, chair of the Department of Dermatology who worked with Shuai (Steve) Xu, an instructor of dermatology at Feinberg and a Northwestern Medicine dermatologist. “The technology has been developed so you can do imaging with the sensors in place and continue monitoring the baby.”
"We were able to reproduce all of the functionality that current wire-based sensors provide with clinical-grade precision."
Saving “Incredibly Fragile” Skin
The blood pressure cuff isn’t the only potentially damaging aspect of current technology. As noted earlier, the sticky tape used to adhere wired sensors to the body can cause skin irritation, blisters, and infections. In some cases, this damage can lead to lifelong scarring.
“Premature babies’ skin is not fully developed during the first weeks of life, so it’s incredibly fragile,” Paller says. “In fact, the thickness of the outer layer of skin in very premature infants is greatly reduced. The more premature you get, the more fragile the skin becomes. That means we have to be very careful.”
So far, the Northwestern team has found no sign of skin damage from the wireless sensors. The sensor’s skin-saving secret lies in its lightweight nature, thin geometry, and soft mechanics.
Developing a New Design

To come up with an optimal design, Rogers worked with longtime collaborator and stretchable electronics and theoretical mechanics expert Younggang Huang, Walter P. Murphy Professor of Mechanical Engineering and Civil and Environmental Engineering, and his group.
To meet the sensor system’s requirements, the team developed flexible and stretchable near field communication antennas to ensure transmission of signals. They also designed substrates to ensure that the babies could not feel the sensors and developed electrodes that minimize the disturbance to the magnetic field associated with MRI scanning.
Though Huang and Rogers had worked together previously to design stretchable electronics, the electromagnetic systems needed for these new patches proved more difficult to design because they were more likely to suffer from electronic degradation when bent or stretched.
The final result was a paper-thin device made from biocompatible, soft elastic silicone that embeds a collection of tiny electronic components connected with spring-like wires that move and flex with the body. The wireless sensor communicates through a transmitter placed beneath the crib’s mattress. Using radio frequencies with the same strength as those used in radio frequency identification tags, the antenna transmits data to displays at the nurses’ station.
"We hope that eventually this device can work not only for babies, but for anybody who needs special medical treatment."
“The problem was fairly complex, involving many aspects of design,” Huang says. “We hope that eventually this device can work not only for babies, but for anybody who needs special medical treatment.”
The device is also cost effective. Although it can be sterilized and reused, the cost of the sensor is so low — about $10 — that it can simply be discarded after 24 hours and replaced with a new one to eliminate any risk of infection.
When Wireless Sensors Go Mainstream
With support from two major nonprofit organizations, Rogers’s team will send sensors to the families of 20,000 infants in India, Pakistan, and Zambia later in 2019. Rogers estimates that his wireless sensors will appear in hospitals in the United States within two to three years.
The next step could be sending sensors home with parents, so they can continue monitoring their newborns after they leave the hospital. The technology could play a role in better understanding and even preventing SIDS — sudden infant death syndrome — the leading cause of death of babies in the first year of life.
“Most parents get even more nervous when their baby is released from the NICU,” Rogers says. “They’re at home then and don’t have monitoring capabilities. Deploying these devices in the home is certainly a possibility and could help parents feel more empowered.”
